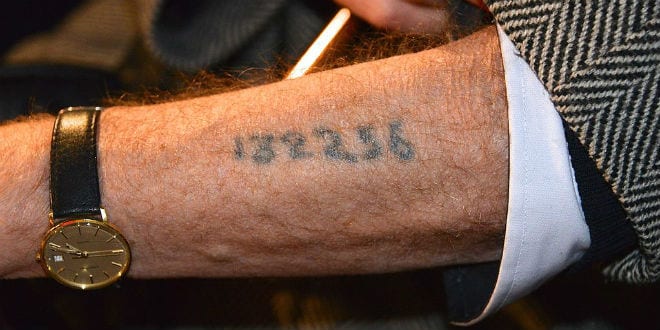“Never Forget!” has long been the axiom when referring to the Holocaust among Jews – and some sympathetic non-Jews – around the world. Yet, sadly, there are thousands among the dwindling number of Holocaust survivors who have forgotten almost everything in their lives – because they suffer from Alzheimer’s disease or other types of dementia.
There will be no more Holocaust survivors left
Of the estimated 200,000 Jews living in Israel who survived the Nazi era in concentration and labor camps, in hiding or elsewhere throughout Europe and some other parts of the world, the average age is 87. Many of them pass away every month, especially since the COVID-19 pandemic began. It is estimated that in a few years, there will be no more Holocaust survivors left in this country to serve as personal witnesses of the horrendous events, although Yad Vashem – the World Holocaust Remembrance Center in Jerusalem – will remain forever as a museum and active monument to the Six Million Jews who were murdered by the Nazis and the minority who survived.

Who remembers survivors who now suffer from drastically reduced cognitive function? Some have children and other relatives, but others are absolutely alone, living in geriatric facilities. One of them is Jerusalem’s 127-year-old Herzog Hospital, Israel’s foremost center for geriatric, respiratory, mental health and psychodrama care, treatment and research.
Research on pressure ulcers
Prof. Efraim Jaul, director of the hospital’s geriatric skilled-nursing department, has much experience with Holocaust survivors, including his own mother, who was born in Hungary, separated as a teenager from her mother by the infamous Dr. Josef Mengele (who sent her to the gas chambers). Fortunately, she was liberated by the British Army at the Bergen-Belsen concentration camp. His father fled Austria in 1939 and moved to Mandatory Palestine, where he joined the British Army; his parents were murdered by the Nazis. Jaul’s father searched in Europe for the young woman to whom his brother had been engaged to marry, but he learned that she had been killed. Instead. He met a woman whom he eventually married and gave birth to Jaul after they settled down together in the State of Israel.
The shortcode is missing a valid Donation Form ID attribute.
A professor at the Hebrew University Medical Faculty, Jaul has written numerous books and conducted research on pressure ulcers, traveling by seniors and end-of-life issues in addition to treating his patients at Herzog.
Protecting one’s level of cognition
He recalled that his mother had a severe stroke at the age of 73 and died at 86. During his childhood, no mention was made of the Holocaust – a common phenomenon in survivors’ families at that time. Either they wanted to try to forget their traumatic experiences, or they were ashamed, or native Israelis didn’t want to hear about the horrors as they fought wars and built up their nascent state.
“If one is fortunate enough to find meaning in one’s life, there is a greater chance of avoiding depression and protecting one’s level of cognition,” Jaul told Israel365. His mother was one of them.
Survivors are more likely to suffer from depression
Thousands of patients have passed through the doors of his geriatrics department, but he always tries to find out from a department nurse or relatives if each admitted patient is a Holocaust survivor. He admits to devoting some extra time and being especially empathic with such people. I try to talk to them about their lives if it doesn’t upset them.”
There are researchers who maintain that Holocaust survivors are more likely to suffer from depression, post-traumatic stress disorder (PTSD) and dementia in their last years than those who did not escape from the Nazis’ clutches because they are more vulnerable and due to what they endured. Others argue that survivors are less likely to have depression or Alzheimer’s disease because survivors were especially resilient and defiant in their efforts to prove that the Nazis were defeated in their quest to annihilate the Jewish People.
Alzheimer’s disease constitutes 60% to 80% of all dementias
“What is old age? It is physical changes, vulnerability, because the body is less able to cope with disease and weakness. So, during one’s life, one can fight physiological decline – exercising your body regularly, eating nutritious food, maintaining healthy weight and exercising your mind – so one doesn’t develop pathology,” Jaul explained.

Elderly with uncontrolled diabetes are at high risk of developing Alzheimer’s disease, which constitutes 60% to 80% of all dementias (other factors are B-vitamin deficiency and clogged blood vessels in the brain), he continued. You can stimulate the mind with intellectual pursuits, being active and curious, playing games, reading and even doing sudoku puzzles to reduce your risk. This increases the number of neural synapses. But there is no recipe for avoiding dementia, Jaul points out.
The physical, cognitive and emotional state of the elderly
“Cognitive decline is multifactorial, including a lack of nutritious food as a child, genetics, lifestyle, chronic diseases and more. Having personally lived through the Holocaust is the most traumatic experience one can have, and it often results in PTSD. But whether one gets dementia partially depends on one’s personality, outlook on life and how you managed after you were liberated. Chronic stress and loneliness are major contributions to cognitive decline,” the geriatrics specialist said. “I don’t think that the Holocaust was a major factor in causing dementia. Stress and trauma that continued for years and a lack of sleep can, however, cause a decline in memory.”
Herzog Hospital includes outpatient clinics that assess the physical, cognitive and emotional state of the elderly. Three rehabilitation departments there treat patients, offer physical therapy and occupational therapy, who then go home, but about two-thirds are brought to the wards for end-of-life care; and patients die, on average, within three months of their arrival. “In general, women are stronger, but they complain more than men. If married, men last longer because their wives take care of them. Women who are alone are less likely to take care of themselves,” noted Jaul.
The shortcode is missing a valid Donation Form ID attribute.
Developing dementia at a rate 1.21 times higher
Previous studies have suggested that compared to the general population, Holocaust survivors are prone to increased risk for PTSD, schizophrenia, cancer, high blood pressure, metabolic syndrome and heart diseases even decades after World War II. The association between exposure to the Holocaust and later-life brain health is limited, but it is well established that late-life cognitive decline may stem from early-life adversities, such as stress, parental death and food deprivation.
A University of Haifa study of 10,000 elderly in 2019 by Dr. Arad Kodesh, Prof. Itzhak Levav and Prof. Stephen Levine that was published in the Journal of Traumatic Stress found that those who were exposed to the traumatic events of the Holocaust develop dementia at a rate 1.21 times higher than those who had not been exposed.
Ghetto survivors had poorer global cognitive performance
Another study from the University of Haifa, Israel Center for Disease Cotro, Tel Aviv University and Rambam Medical Center that appeared recently in the Journal of Psychiatric Research, entitled “Holocaust exposure and late-life cognitive performance in men with coronary heart disease,” looked into the question of whether Holocaust victims who experienced extreme physical and mental stress could when very old, suffer prolonged deficits in psychological and physiological well-being. They examined specifically whether exposure to Holocaust conditions was associated with cognitive function and decline in a sample of elderly male adults with coronary heart disease.

Drs. Galit Weinstein, Miri Lutski, Lital Keinan-Boker, Uri Goldbourt and Prof. David Tanne studied 346 elderly with coronary heart disease and a mean age of 71.8 years: Forty-three of them survived concentration camps/ghettos, 69 were Holocaust survivors who escaped concentration camps/ghettos, and 234 (68%) were not Holocaust survivors. The researchers found that concentration-camp/ghetto survivors had poorer global cognitive performance and poorer attention compared to those who were not exposed to Holocaust conditions. Additionally, participants who reported being at concentration camps or ghettos had increased cognitive decline in global performance and executive function compared those who were not Holocaust survivors. Lastly, those who were Holocaust survivors but not in concentration camps/ghettos had a greater decline in attention.
Cannot be proven with absolute certainty
But other researchers say this cannot be proven with absolute certainty, as these studies did not look at the entire gamut of survivors but only those who lived in Europe; and that they examined those who lived longer and contracted dementia (which many non-Holocaust survivors also develop) and not those who died at younger ages.
Still, it is incontrovertible that survivors at the end of their lives, whether they suffer from dementia or are still cognitively aware, are not getting enough financial and emotionally supportive help from the Israeli government and its institutions. Additionally, the loneliness forced upon them by the COVID-19 pandemic has exacerbated their condition.
The shortcode is missing a valid Donation Form ID attribute.