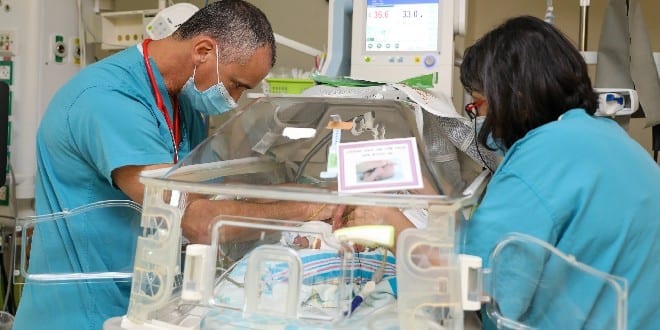
For several decades, very-premature babies born at the age of 24-to-34 weeks (out of the full-term of 40) were saved in hospital intensive-care units by invasive intubation (insertion into the windpipe) with thick and rigid tubes for introducing into their underdeveloped lungs air or an air/oxygen mixture under pressure.
But some pediatricians have argued that such a procedure, which could cause even serious damage to the delicate nasal tissues of such tiny infants, was unnecessary. Nobody conducted serious research to decide the controversy – until now when physicians at Rambam Medical Center in Haifa have completed a conclusive and groundbreaking study on the matter.
The study is well-timed, as Israel Premature Baby Day is marked annually on November 24th.
Dr. Ori Hochwald, Dr. Arieh Riskin, Dr. Amir Kugelman and Dr. Liron Borenstein-Levin, in collaboration with Bnei Zion Medical Center in Haifa, have brought to an end the controversy that has existed for years in preterm medicine: Are nasal prongs with thick tubing introduced into the tracheas preferable to thin cannulas in the noses of preterm infants who require intermittent positive-pressure ventilation? Their findings for the first time provide answers that could change the way preterm infants are treated in medical centers around the world.
This first clinical study of its kind, conducted by the Haifa researchers, presents new data that prove preterm infants can be ventilated effectively and without damaging their delicate faces. The study was just published in the prestigious scientific journal JAMA Pediatrics under the title “Cannula with Long and Narrow Tubing vs Short Binasal Prongs for Noninvasive Ventilation in Preterm Infants – Noninferiority Randomized Clinical Trial.”
The prevailing opinion among physicians was that the use of rigid tubes allows for better transfer of air pressure and support to preterm infants, compared to the use of thin tubes,” explained Hochwald, a senior pediatrician in Rambam’s premature baby unit who headed the study. “In some cases, the preterm infants who had the thick tubes in their noses suffered significant injuries that would have taken some time to heal.”
The randomized clinical trial included 166 preterm infants at 24 to 34 weeks gestation who needed positive-pressure ventilation. From the processing of the preterm infants’ data, it emerged that in the respiratory group using the thick tubes, which is commonly used in preterm infants around the world, the success rates of the treatment according to the established criteria were 82%. The second group, the one used in the thin tubes (the new method), showed a success rate of 86%, according to the same criteria, and with a significantly lower percentage of injury in the patients’ noses. “Our intention was to prove that the new, more gentle method is no less effective than the prevailing method,” said Hochwald.
“It sounds like something minor, but for doctors, infants, and their families, the findings allow for a significant improvement in preterm care,” he conducted. “To this day, many pediatricians were unwilling to use this method because they thought it was less effective. Now there is proof. Since we are talking about a treatment that most preterm infants will receive at one time or another, this is an important step for everyone.”
The shortcode is missing a valid Donation Form ID attribute.